Microbiome Basics
Microbiome basics, inflammation, and why this system quietly shapes your health
J Shore, K Kulifay
3/16/20264 min read
Microbiome basics, inflammation, and why this system quietly shapes your health
Most people think of the gut as a food processor.
Food goes in. Nutrients come out. End of story.
But your gut is less like a machine and more like a living ecosystem. It is constantly sensing, responding, protecting, repairing, and communicating with the rest of your body. It helps regulate immunity. It helps control inflammation. It influences metabolism. It even plays a role in how resilient you feel day to day.
In many ways, your gut is not just part of your health.
It is one of the systems helping coordinate it.
The microbiome: your internal ecosystem
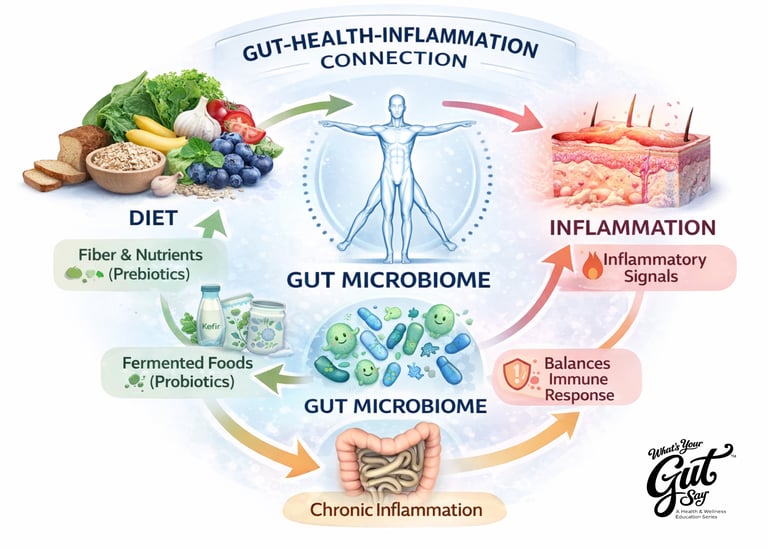
Inside your digestive tract lives a vast community of bacteria known as the gut microbiome. These organisms are not just passive passengers. Many play active roles in helping your body function. They assist in breaking down certain foods, producing vitamins, maintaining the gut lining, and helping your immune system decide what is harmless and what might require attention.
When this internal ecosystem is relatively balanced, the body tends to operate with more stability. When it becomes disrupted, a state researchers call dysbiosis, the effects may begin to show up in ways that are not always obviously connected to digestion.
Researchers are increasingly studying how microbiome imbalance may relate to inflammatory patterns, immune regulation, metabolic health, and other long-term wellness factors. This does not mean the microbiome explains everything. Health is always influenced by multiple systems. But it does mean the gut is more foundational than we once thought.
A helpful way to think about the microbiome is as a garden.
When the soil is diverse and supported, beneficial organisms tend to flourish and keep the environment stable. When the environment becomes depleted or repeatedly stressed, less helpful organisms can begin to dominate. Gut health often follows a similar pattern. It is less about perfection and more about what conditions you create over time.
Inflammation: your body's repair system
Before trying to reduce inflammation, it helps to understand what it actually is.
Inflammation is not a mistake. It is part of your body’s repair strategy.
When something irritates or injures tissue, the immune system increases blood flow and sends repair signals to that area. This is why inflammation often shows up as swelling, redness, warmth, or tenderness. These are signs that your body is trying to protect and repair itself.
In the short term, this process is both normal and necessary. It helps cuts heal. It helps the immune system fight infection. It even plays a role in how muscles rebuild after physical activity.
The concern is not inflammation itself. The concern is when the body remains in a low-grade inflammatory state for long periods of time.
If acute inflammation is like calling the fire department when there is smoke, chronic inflammation is like leaving the alarm system stuck in emergency mode even when nothing is actively burning.
Over time, this persistent background inflammation may influence digestion, immune regulation, metabolic health, skin stability, hormone signaling, and energy levels. It often does not announce itself dramatically. Instead, it tends to show up as patterns that feel subtle at first but persistent over time.
This is one reason gut health has become such an important conversation in preventative health.
Why the gut influences inflammation so strongly
A large portion of immune activity occurs in and around the digestive system, where the body is constantly evaluating what should be absorbed and what should be treated cautiously. Every meal represents a negotiation between the outside world and your internal environment.
When the gut environment is supported, this system tends to stay calm and regulated. When it is repeatedly stressed, through low fiber intake, highly processed food patterns, chronic stress, disrupted sleep, or illness, the immune system may become more reactive. This may contribute to increased inflammatory signaling beyond the digestive tract.
Because of this, researchers are now examining gut health in connection with immune resilience, metabolic stability, hormone balance, skin health, and neurological function. The gut does not control everything, but it participates in far more than we once realized.
Prebiotics and probiotics, without the confusion
Much of the discussion around gut health focuses on prebiotics and probiotics, but the basic concepts are actually straightforward.
Prebiotics are the nutrients that beneficial gut bacteria feed on. Most commonly, these come from certain plant fibers that your body cannot fully digest but your microbiome can. You can think of prebiotics as the fuel that keeps beneficial bacteria active.
Foods naturally rich in these fibers include onions, garlic, oats, apples, bananas, asparagus, and legumes. In most cases, increasing plant diversity in your diet naturally supports this process without requiring specialized products.
Probiotics, by contrast, are live microorganisms found in fermented foods and certain supplements. Yogurt with live cultures, kefir, sauerkraut, kimchi, and similar foods are common sources.
What is important to understand is that simply consuming live bacteria does not guarantee meaningful change. Researchers are still determining which strains survive digestion, which remain active, and which may be helpful in specific contexts. Some show promise in certain situations, while others appear to have limited measurable effect.
This is why the fundamentals, overall diet quality, sleep, stress regulation, and consistent lifestyle patterns, remain far more influential than any single supplement.
Anti-inflammatory eating as a foundation, not a trend
Once inflammation is understood as a biological process rather than a marketing term, anti-inflammatory eating becomes much easier to understand. It is not a restrictive diet. It is simply a pattern of reducing inputs that repeatedly stress the body while increasing those that support stability.
Across decades of nutrition research, similar themes continue to appear. Diets emphasizing whole foods, plant diversity, fiber, and healthy fats tend to support metabolic and gut health more consistently than diets dominated by ultra-processed foods and excess refined sugars.
This is one reason Mediterranean-style eating patterns are frequently referenced in research. These approaches naturally emphasize vegetables, fruits, legumes, nuts, seeds, olive oil, fish, and minimally processed foods while lowering the constant inflammatory pressure associated with excess sugar and heavily processed ingredients.
Importantly, this is not about strict adherence. It is about improving the overall pattern.
Your gut responds to consistency not perfection.
The real takeaway
Gut health is rarely determined by one food, one supplement, or one decision. It is shaped by the conditions you create over time. Feeding beneficial bacteria through fiber, introducing microbial diversity through fermented foods when appropriate, and reducing the constant pressure of ultra-processed dietary patterns all help create a more stable internal environment.
In many ways, supporting your gut is less about fixing something broken and more about creating conditions where your body can function the way it was designed to.
Because the gut is not just reacting to what you eat, it is responding to the pattern of how you live.
